“Thought I’d Lose Her”: Doctor Shares Long Journey of Saving Pregnant COVID-19 Patient
Dr Vikas Maurya, Director and Head of Department, Pulmonology, Fortis Hospital, shares his experience of the second wave and the perils doctors face in the COVID ward.

In January 2020, when news of SARS-CoV2 trickled into India, the medical fraternity was just trying to understand the virus and how it would impact the infected. There was hardly any data, and China, the country from where the virus originated, was under a clampdown.
From then until March 2020, I was gathering as much information as possible on the virus and focused on disseminating the knowledge to people who are at a higher risk of getting infected. I had started conducting lectures in various places, which included police stations, hotels and even other hospitals in the city. These lectures were focused on how to prevent the virus from spreading and creating a general environment of awareness about SARS-CoV2. I knew that it was only a matter of time before it would hit us, but I never imagined it would be like a tsunami that would engulf us without any life support.
When the nation-wide lockdown was announced, there was trepidation of what was to come. When China reported 80,000 cases, I had assumed that we, in India, would have maybe double the cases and anticipated about 1 lakh cases. However, the number of cases that we started seeing was not something I, or others in the medical fraternity, were ready for.
After weeks of hard fighting, we got through the first wave and heaved a sigh of relief. But even before we could fully settle down into our normal routines, the second wave was upon us. This time, it was even more overwhelming than the first wave, given that the sheer volume of cases had increased tremendously. What was also different about the second wave was that we were seeing so many more young patients and some pregnant women. COVID in pregnant women is even more dangerous. When you are pregnant, your abdomen is distended and the lungs are already in a compromised situation. In such cases, even a moderate infection can turn into a severe one rather quickly.
The wave was so rapid and huge that we had close to 250 COVID patients being treated in the hospital at any given time.
It was nothing short of a war zone. There were COVID patients everywhere and almost every patient needed to be put on ventilator support. We bought, and even borrowed, ventilators and were still falling short. The hospital added as many ICU beds as they possibly could. Such a situation was not something that we had ever anticipated or were prepared for.
The amount of pain and pathos that I witnessed during the second wave is something that will not leave my memory anytime soon. In my over two decades of experience, COVID-19 is one that has brought so much loss and anguish. Like everyone else, even I have lost friends and colleagues to the virus. Sometimes, I didn’t even have time to grieve their loss, I just had to pick up the pieces and move on.
I have encountered families during my tele-consult who had given up on finding a hospital bed and getting access to oxygen. They would just plead with me to take on the case virtually and treat them in the best possible manner. It was so heartbreaking. Even those who found a bed in the hospital would be weeping when we went on our rounds. It was like they were all chanting together to be saved or helped out of the situation.
COVID-19: A ‘Blessing in Disguise’
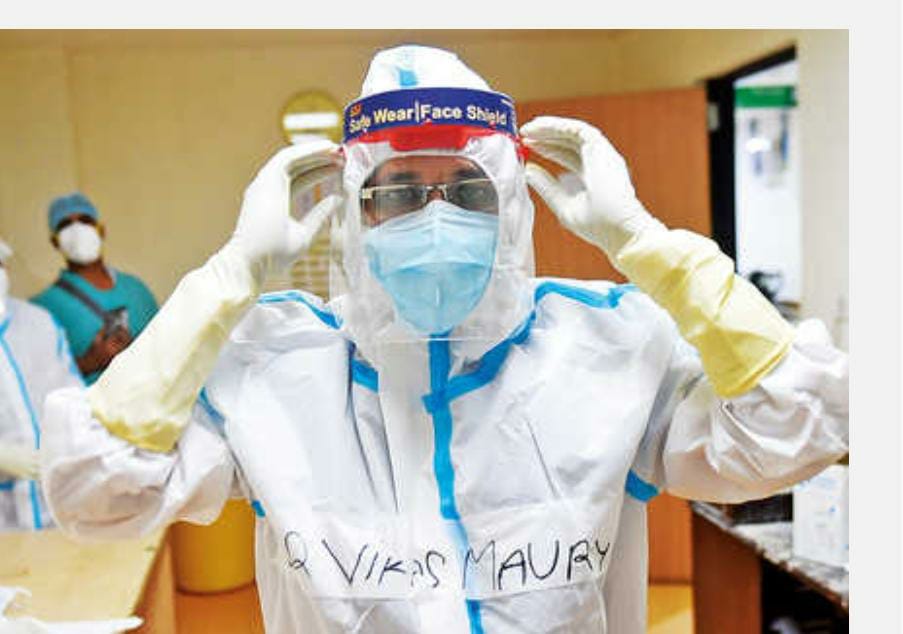
Despite having treated patients in the first wave and having been vaccinated, during the second wave I also got COVID-19.
I was leading the COVID care in the hospital, and even though I had contracted COVID-19, I could not afford to take a day off. I took a room in the hospital and while I thought I would be fine in two days, things deteriorated on the third day and I had to be admitted.
The infection had reached my lungs. I was also put on the regular treatment protocol to fight it. It took me five days to get better, so rather than going home, I decided to stay back and continue my work. With an IV cannula in my hand, I would go around and complete my rounds. With so many of the doctors and frontline workers falling sick, I could not afford to take time off.
Contracting COVID-19 was, in a way, a blessing in disguise. It meant I could go around the COVID ward without the PPE kit. This allowed me to work faster and see more patients. And since I tested positive, there was no fear of the virus either. I felt almost emboldened. In between all this, my wife and two kids [aged 8 and 11] also tested positive. Here I was treating my patients and also doing tele-consults for my own family who were isolating at home.
‘Even we are human beings at the end of the day.’

As a doctor, I am trained to be dispassionate, but among so many cases, there were a few, which really made me emotional. One patient in particular, who was not only difficult to treat but also left me emotionally drained, was a 32-year-old lady who happened to be six months pregnant when she contracted COVID-19. She came to me as a severely impacted patient with acute pneumonia as well. We had to work hard to save her and the baby as well. It was a high risk case. I remember my initial thoughts when I saw her — the fear of losing her was looming large.
Everything that could go wrong was happening to her. She was brought to the hospital at a stage when the infection had already spread and compromised her lungs. She needed 100 per cent oxygen support and eventually had to be put on a ventilator. That was a very distressing moment for me as her doctor. It almost felt like a state of helplessness. Her body was not reacting to any treatment protocol. While we started with the lowest possible treatment options, we soon had to ramp it up, given that she was not responding to any treatment.
This patient was also experiencing ARDS (Acute Respiratory Distress Syndrome), which occurs when fluid builds up in the alveoli [tiny, elastic air sacs] in your lungs. The fluid keeps your lungs from filling with enough air, which means less oxygen reaches your bloodstream. This deprives your organs of the oxygen they need to function.
We also faced a lot of limitations. For example, we could not get an X-ray done daily or even try the prone position when the oxygen saturation levels dipped.

I had to do a lot of research in order to be 100 per cent sure of the treatment protocol for her. What really helped was having her supportive family back every decision of mine. Truly speaking, my first responsibility was towards the lady, I knew I had to save her. The baby would follow.
But she was on the ventilator for a long time, none of the treatment worked, she was in sepsis and even her blood pressure levels were skyrocketing. She even contracted bacterial pneumonia and had to undergo bronchoscopy and tracheostomy.
However, every small recovery of hers motivated us.
My team fought without ever giving up, and the patient also fought hard – not just for her life but for her child as well. Slowly but surely, her health took a turn for the better after close to a month in the hospital. I remember the day she was discharged – I almost felt like I had held on to my breath until that moment.
Ensuring that both the mother and the baby survived the ordeal was the best feeling ever. Such moments make all the stress and exhaustion worthwhile.
The second wave was something else, and we, as doctors, did everything in our control to keep the situation manageable. This is my profession, I signed up for this and I am proud of each and every frontline worker.
– Dr Vikas Maurya, Director and Head of Department, Pulmonology, Fortis Hospital Shalimar Bagh As Told To Vidya Raja
(Edited by Yoshita Rao)
If you found our stories insightful, informative, or even just enjoyable, we invite you to consider making a voluntary payment to support the work we do at The Better India. Your contribution helps us continue producing quality content that educates, inspires, and drives positive change.
Choose one of the payment options below for your contribution-
By paying for the stories you value, you directly contribute to sustaining our efforts focused on making a difference in the world. Together, let’s ensure that impactful stories continue to be told and shared, enriching lives and communities alike.
Thank you for your support. Here are some frequently asked questions you might find helpful to know why you are contributing?


This story made me
-
97
-
121
-
89
-
167











