Band of Doctors Sets Up Makeshift COVID-19 Hospitals That Treat Thousands for Free
When COVID-19 cases touched 90,000 in July in Delhi, doctors converted the Commonwealth Stadium into a 500-bed hospital in a week.

It has been nearly 24 hours since Dr Ravikant Singh has slept and his phone is buzzing non-stop. Patiently, he returns each call and comes up with a way to solve various problems – from his team member catching COVID-19, a lack of PPE kits to getting a signature from a government official.
Dr Ravikant may not remember the last time he ate a proper meal but he surely knows the exact number of COVID-19 patients in makeshift centres built by his organisation, ‘Doctors For You’ (DFY), in 12 states to provide free treatment.
After doing his rounds in the makeshift COVID-19 centre in Patna, where he is currently stationed, he quickly calls an ambulance driver in Mumbai to check if he is recovering well from the deadly virus.
Every inch of his body aches and his fingers and toes feel numb due to the suffocating PPE kit, but that has not wavered his dedication towards patients.
It has been six months since he has been juggling between setting up makeshift centres along with the various state governments and managing his team of over 500 frontline health workers across India.
The never-ending chaos is not new to Dr Ravikant as he has already served in over 25 disaster relief operations since 2007 by setting up makeshift clinics.
He established DFY primarily to help vulnerable communities during disaster situations like floods and epidemics by providing emergency medical aid. It partners with organisations like UNICEF, private organisations and governments to carry out capacity building in emergencies.
From riot-hit Assam, the Nepal earthquake to flood-affected Chennai, the DFY team comprising doctors, nurses, medical students and paramedics have saved thousands of lives and resources with their quick and innovative setups in the middle of havoc.

“Every disaster severely cripples the economy and uproots thousands of lives. The rehabilitation process takes weeks and sometimes months. I saw this during the deluge of Mumbai when I was a medical student at KEM hospital. The local administration is always in dire need of medical staff. As a doctor, it is my duty to save lives outside my antiseptic wards also and with this idea, DFY was born. I have never seen anything like this pandemic before and we thought our expertise in disaster operations could be useful. The COVID-19 vaccine is far away but until then we need enough hospital beds,” Dr Ravikant tells The Better India.
Setting up Make-Shifts Centre for Free COVID-19 Treatment

Dr Ravikant says DFY is presently managing nearly 2000 beds that come with oxygen cylinders, ventilators, toilets, waste incinerators, doctors and nurses. Each person works in 6-hour shifts and 15 medical personnel are kept as a backup in every centre.
Doctors, nurses, ambulance drivers and paramedics are hired on contract basis for a minimum period of three months and they also welcome volunteers. All their hired staff is below 35 years of age as they are less prone to the virus.
It takes a minimum of two weeks to identify and set up the clinics as per the state guidelines. Things move quickly if it is an already established facility like the Commonwealth Games (CWG) Stadium in Delhi that already has air conditioning, toilets and enough space to accommodate doctors and nurses.

“A major challenge is to build toilets. We have to keep it sanitised at all times. Every admitted patient stays at least for two weeks and we have to look after their food and bathing. In Delhi, we rejected three halls because of unsanitized toilets. We build our centres in a way where every toilet and ward is separate for men, women and children to avoid any kind of women or child-related crimes,” says Dr Ravikant.
As architects and engineers build the centre, the medical staff undergoes mock drilling on how to handle patients, maintain social distancing, avoid panic and things to do in case of lack of medical equipment.
DFY’s timely response and years of experience certainly came handy when COVID-19 cases in Delhi touched 90,000 in July.
The mammoth task of turning the stadium into a COVID-19 facility with 500 beds was completed in less than a week.

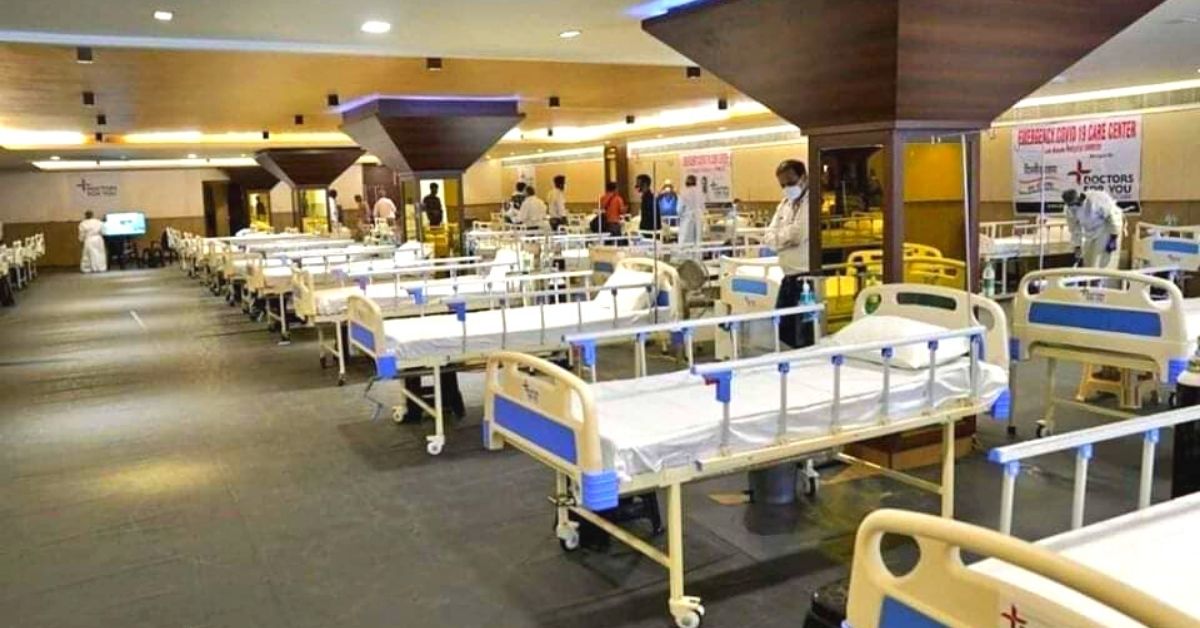
“We converted the central badminton and table tennis hall. Most beds are attached with oxygen supply and patients are monitored via CCTV. There are 80 makeshift toilets for the patients and 30 bathing areas. For every 30 beds, there is one doctor and two nurses working on shifts. A separate area is just for doctors and nurses to rest and eat their food. Impressed with the staggering feat, the state government permitted DFY to convert a banquet hall,” says Dr Shailender stationed at the stadium.
If the centres experience heavy traffic in patients, instead of turning them away, the organisation starts discharging patients who are on the road to recovery and directs them for home isolation.
One of the biggest takeaways in setting up the centres is to have a 100 per cent commitment from the state governments in terms of ensuring steady cash and medical equipment flow.

“Our staff is the backbone, so if they suffer in terms of salary or safety gears, it affects the overall situation. They are putting their lives in danger every day so cannot tolerate delayed salary payments or any such issue. Only after the state government commits on paper, do we sign the contract. Fortunately, all the states have been very cooperative and supportive,” says Dr Ravikant.
DFY offers three types of centres, for mild, moderate to severe patients and the cost differs for each. The daily average cost, that is borne by the government, per patient is Rs 4,000 and if the person has to be shifted to ICU then it touches Rs 12,000. Even the machines cost several lakh.
“The overall expenditure can range from Rs 40,000 to Rs 10 Lakh. Just the gown costs Rs 1,000, and that is used only once. Money is a very crucial factor if we have to build a quality care centre. In some places, we had to spend more on PPE kits than the salary of our staff,” he says.

The high-standard facility and services provided by DFY have encouraged several health workers to extend their contract. Sonu Sharma, Nursing Officer at CWG stadium, is one such nurse.
The 29-year-old was stationed in July and even though it is her first disaster stint, she is not scared and is, in fact, happy that she can help save lives.
“I joined DFY in July and not once have I thought of quitting. The patients have become my family as the facilities are top-notch here including food and accommodation which is rare in a disaster-like situation. We get two days off after every 12-hour shift so that we are not fatigued or over-pressured. I even celebrated my birthday here away from my parents but the patients and co-workers made it special for me. I will work here till every patient is cured, ” Sonu tells The Better India.
Future of COVID-19 in India

According to Dr Ravikant, the coronavirus battle will last at least for two years as even if the vaccine is ready, it will first go to a certain section including health workers, elderly, immuno-compromised people, pregnant women and then to healthy adults and children.
India is reporting the highest daily death and new infections globally and we are struggling to give an effective response. As per one prediction, the world will have two billion vaccines by 2021 so a country with 1.3 billion population will have to wait longer before every person is covered. The next best thing is, thus, to develop a robust healthcare system that can handle the crisis for at least 2.5 years,” he says.
Dr Ravikant further adds that doctors, who are touching and breathing coronavirus daily, cannot alone fight the pandemic. Citizens can tremendously unburden the exercise simply by wearing masks and maintaining social distancing.
(Edited by Vinayak Hegde)
If you found our stories insightful, informative, or even just enjoyable, we invite you to consider making a voluntary payment to support the work we do at The Better India. Your contribution helps us continue producing quality content that educates, inspires, and drives positive change.
Choose one of the payment options below for your contribution-
By paying for the stories you value, you directly contribute to sustaining our efforts focused on making a difference in the world. Together, let’s ensure that impactful stories continue to be told and shared, enriching lives and communities alike.
Thank you for your support. Here are some frequently asked questions you might find helpful to know why you are contributing?


This story made me
-
97
-
121
-
89
-
167











