TBI Blogs: Do You Suffer from Cancer, Diabetes, Etc.? India’s New National Health Policy Is Great News for You
The Ministry of Health & Family Welfare recently passed the National Health Policy, 2017. Dr. Kenneth E. Thorpe takes a look at how the Policy’s new focus on non-communicable and chronic diseases will help overhaul India’s healthcare policy for the better.
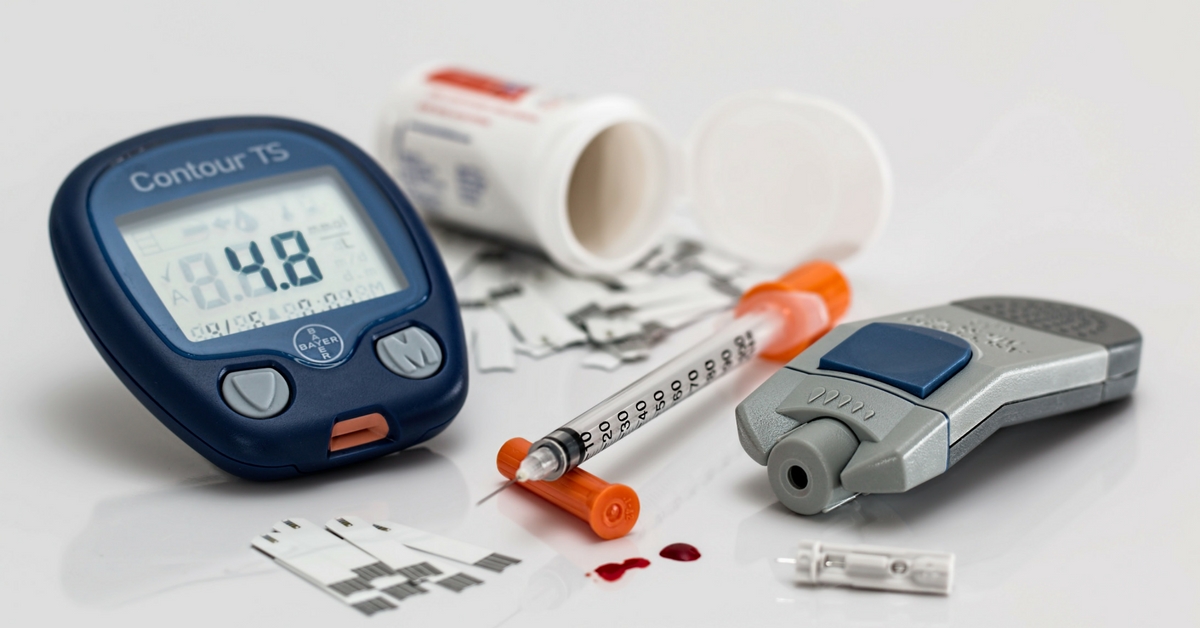
The Ministry of Health & Family Welfare recently passed the National Health Policy, 2017. Dr. Kenneth E. Thorpe takes a look at how the Policy’s new focus on non-communicable and chronic diseases will help overhaul India’s healthcare policy for the better.
Finally, there is something to cheer about. The government announced the new India National Health Policy 2017 after a gap of 15 years. This policy, announced by JP Nadda, Minister of Health and Family Welfare, aims to ensure that healthcare reaches everyone, particularly the under-served and underprivileged. It has given everyone in the health sector lots of hope, and everyone is optimistic that it will be able to address the current and emerging challenges necessitated by the changing socio-economic, technological, and epidemiological landscape.
The key takeaways
The policy has assigned specific quantitative targets aimed at reduction of disease prevalence/incidence under three broad components—viz.(a) health status and program impact, (b) health system performance, and (c) health systems strengthening—aligned to the policy objectives. All these are signs of a very well-thought out, progressive policy, and we are thankful for that, as there is need for timely intervention now to bring about a noticeable and worthwhile change in the disease map of India, particularly for widely spreading non-communicable diseases (NCDs).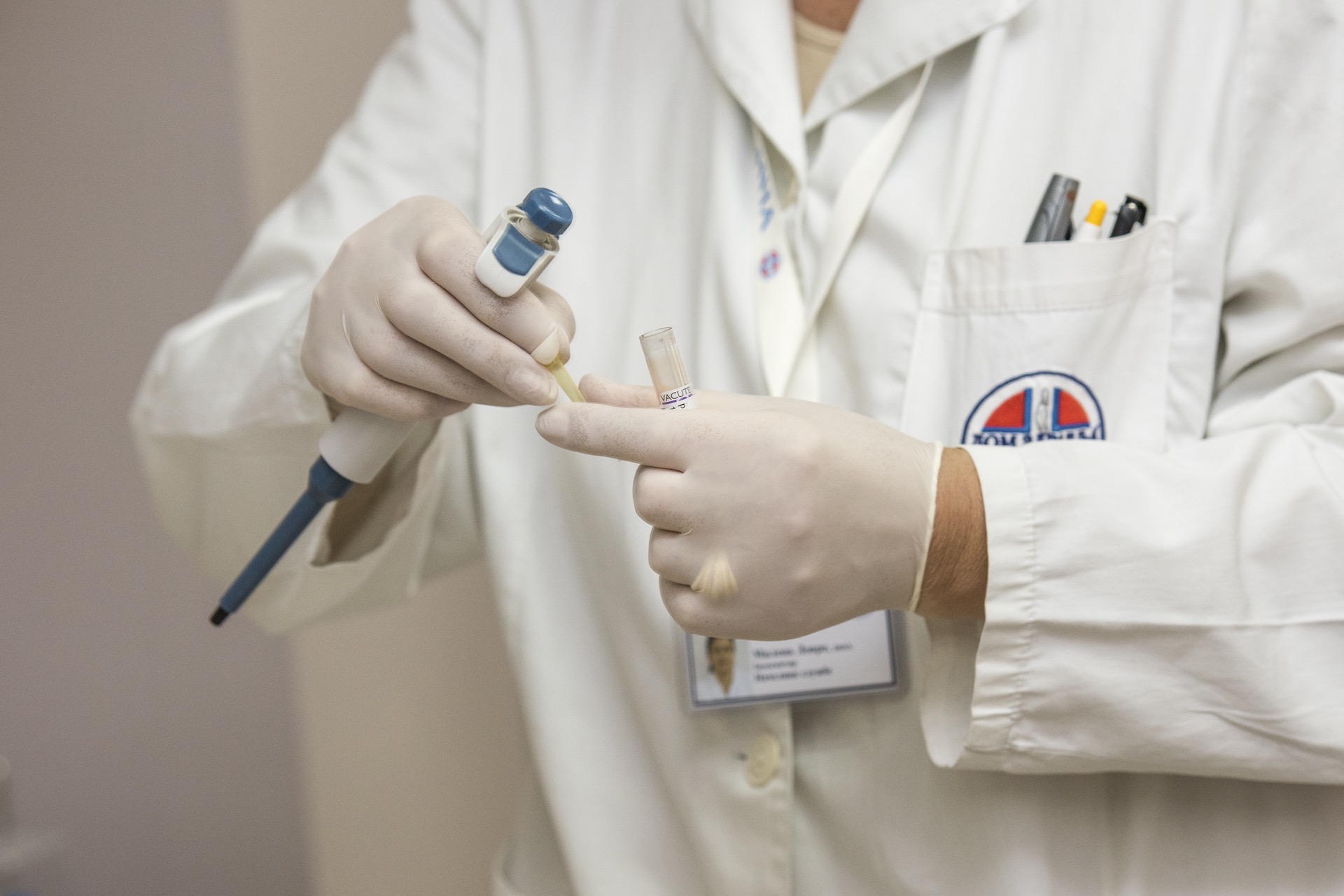
The focus on NCDs
This policy has clear focus on tackling the emerging challenge of non-communicable diseases. The government, it is clear, intends to now play a lead role in providing innovative, sustainable healthcare financing models that enable all Indians to access necessary services for prevention, diagnosis, and treatment of NCDs.
The policy supports an integrated approach, where screening for the most prevalent NCDs with secondary prevention will make a significant impact on reduction of morbidity and preventable mortality. It mentions as one of its aims, “To reduce premature mortality from cardiovascular diseases, cancer, diabetes, or chronic respiratory diseases by 25 % by 2025.” This is indeed a good goal to work toward.
With a good focus on NCDs, the new National Health Policy will be an improvement programme to reach and support citizens with chronic diseases in varied settings. Chronic diseases are among the most prevalent and costly healthcare problems, as well as the most preventable.
Lack of prevention of chronic diseases has impact particularly on the quality of life, escalating healthcare costs, and the overall economy. This policy has given these diseases a preventive approach rather than being curative. What is left to see is whether these prevention programmes are appropriately tailored to specific populations.
When directly tied to particular interventions or population groups, prevention can be cost-effective, even in the short term.
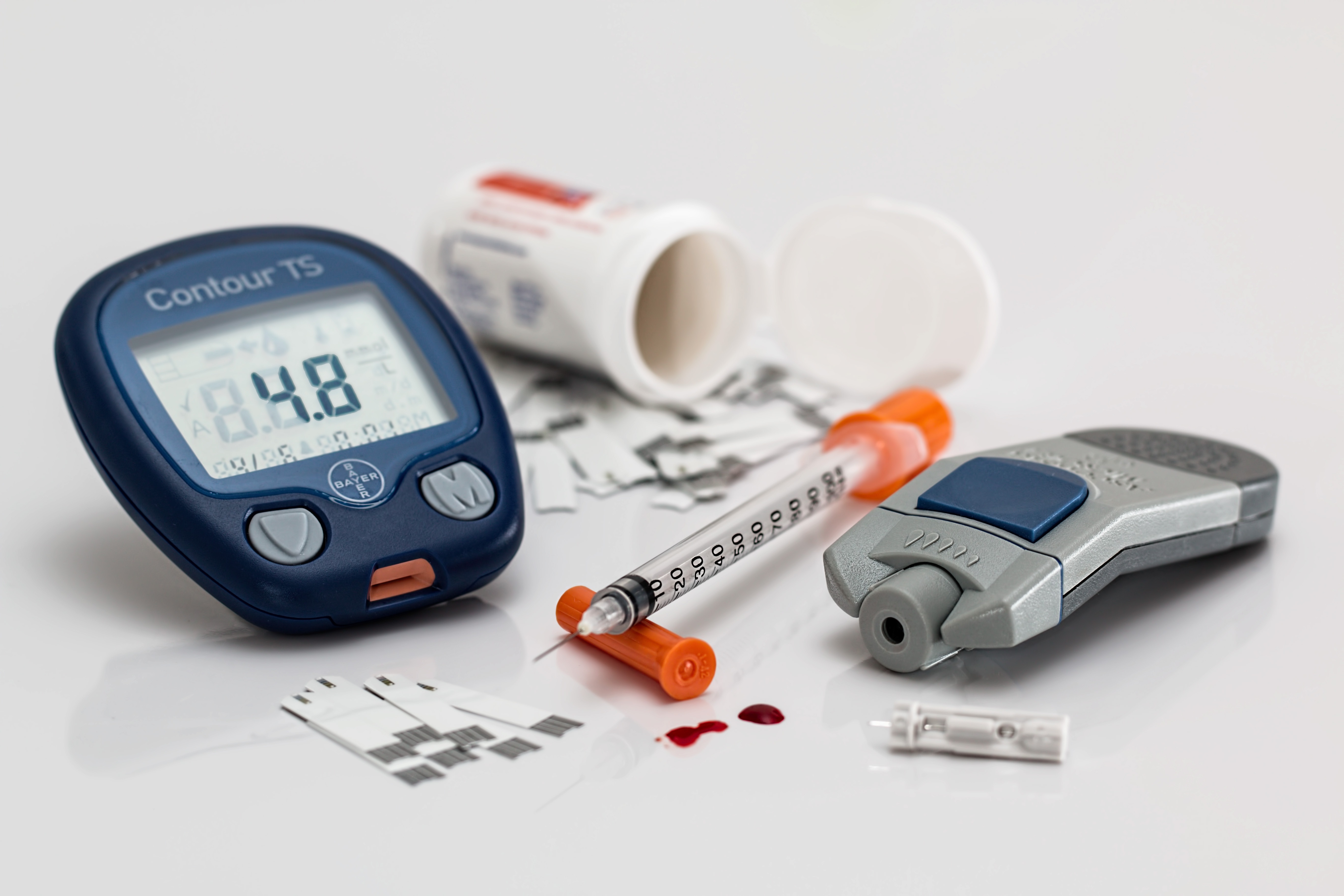
The policy recognizes the interplay of the three thematic tracks presented in the national NCD blueprint SANKALP brought out by the Partnership to Fight Chronic Disease (PFCD) in 2015—Policy and Surveillance, Strengthening of Healthcare systems, and Healthcare Financing. PFCD, therefore, looks forward to working with the government to meet India’s healthcare delivery objectives.
Some other measures recommended by SANKALP included strengthening the tertiary tier of hospital-based healthcare, developing the local primary healthcare system to be able to broadly screen and diagnose key diseases, providing extensive diagnostics and free essential drugs, expansion of health insurance through both public and private payers, providing coverage even to those in unorganized sectors, using CSR to further enhance healthcare delivery, and switching focus from patient care to preventive care.
Crucial decisions
It is encouraging to see that the new National Health Policy recognizes the need to raise the healthcare spend by proposing an increase in public health expenditure (through National Health Accounts) from the current 1 % of GDP to 2.5 %. This is a very crucial component of the policy, but only a small step toward achieving the minimal level of public investment in healthcare as recommended by the WHO and other leading health policy experts.
The recognition of expansion insurance as an essential healthcare financing tool was also much needed. We are also hopeful that the policy will enable the growth of private health insurance – through employers and commercial insurance products – and attract more private investment in the healthcare sector.
The National Health Policy advocates a progressively incremental health assurance-based approach. It envisages providing larger packages of assured comprehensive primary healthcare through ‘Health and Wellness Centers’, and denotes important change, from very narrow to a comprehensive primary healthcare package which includes care for major NCDs, mental health, geriatric healthcare, palliative care, and rehabilitative care services.
It advocates allocating a major proportion – two-thirds or more – of resources to primary care.

The recommendations in the National Health Policy suggest sincere consideration to reduce out-of-pocket expenditure through a multi-model approach, using both public and private payers. Efforts to reduce out-of-pocket expenditures will come only if it is done keeping in mind the huge disparity in terms of income, employment, and geography in India, and ensuring a range of options from the public and private sector to expand insurance coverage.
Finally
There’s lots to applaud in the new National Health Policy—increase of spends, preventive care, making provisions for primary healthcare (PHC) facilities and making them robust, prioritization of NCDs, recognizing expansion of health insurance as a necessary means to reduce out-of-pocket expenditures, and achieve universal healthcare coverage. This policy has the power to bring about reforms in the healthcare sector. Now there is need to forge strong partnerships with the private sector to expand the delivery and coverage of healthcare services far and wide across this vast country.
Of course, effective implementation and evaluation are key to realize the potential benefits and intended outcomes of the National Health Policy to improve the health, quality of life, and financial security of the citizens of India.
(The author is the Chairman, Partnership to Fight Chronic Disease. He is also the Robert W. Woodruff Professor of Health Policy at Emory University, Atlanta, Georgia, USA.)
To find out more about NCDs and how you can contribute, contact PFCD India via email or on Twitter.
Like this story? Or have something to share? Write to us: [email protected], or connect with us on Facebook and Twitter.
NEW: Click here to get positive news on WhatsApp!
This story made me
- 97
- 121
- 89
- 167
Tell Us More
We bring stories straight from the heart of India, to inspire millions and create a wave of impact. Our positive movement is growing bigger everyday, and we would love for you to join it.
Please contribute whatever you can, every little penny helps our team in bringing you more stories that support dreams and spread hope.



















