TBI Blogs: This Indian Psychologist Used Interactive Games to Help Children in Tajikistan Fight TB
Dr Ruchi Brahmachari, a clinical psychologist from Mumbai, looks back on her time in Dushanbe, Tajikistan.

Ruchi Brahmachari, a clinical psychologist from Mumbai, looks back on her time in Dushanbe, Tajikistan.
According to the World Health Organisation, Tajikistan is one of 27 high multidrug-resistant TB (MDR-TB, or TB that is resistant to first-line drugs) burdened countries in the world. MSF runs a paediatric TB care programme in the country, providing diagnosis and treatment to children living with TB.
When I was first given the opportunity to go to Tajikistan, I was a bit apprehensive because, although I have worked as a clinical psychologist before, I had never worked with patients living with tuberculosis (TB).
I spent nine months in the capital city of Dushanbe, as part of the mental health team. It was a steep learning curve for me, but I began to pick up the pulse of the project soon.
The treatment for TB is a long and uncomfortable process, and can lead to side effects such as nausea, anxiety, palpitations, headache and gastric issues.
The mental health team’s responsibility is to provide nutritional and psychosocial support to keep patients motivated through the arduous course of treatment.

Photo: Wendy Marijnissen
This includes implementing incentives like rewarding children with a sticker, every time they take their medicine properly.
Since the treatment for MDR-TB can take up to two years, it keeps children from going to school and affects their overall physical and mental development. For example, 4 or 5-year-olds undergoing treatment won’t go to school till they are 6 or 7 years old. We had children in the in-patient unit who couldn’t tell red from yellow, or yellow from blue.
Many of these children also come from very impoverished homes and thus, do not get developmental stimulation even at home.

Photo Credit: MSF
To ensure that a child’s development does not suffer during the course of the treatment, MSF runs a therapeutic play programme for children. The mental health team organises regular group sessions with children involving development stimulating activities, such as storytelling, drawing, handicrafts or games.
These sessions serve as a channel for them to counter the emotional stress of being away from home, deal with the isolation of having lost their parents to TB in many cases and simply know more about how to cope with their illness.

Photo Credit: MSF
One time, we had a group of seven kids between the ages of 1 to 3,in the in-patient unit at the same time. These were children who had begun to walk when they had first come to us but had regressed because of hospitalisation. To get them back to walking, we worked with mothers showing them how to stimulate the child. The tendency for parents is to carry their child because he is sick, so whatever opportunities there are for him to reach his development milestones get further reduced.
Typically, in hospitals, one is always advised that if you are sick, you stay in bed. But for us, it was really important to educate the parents that, ‘if your child has the energy it’s ok for him to go and run about; if he is unwell, he will stop himself.’
I also worked proactively on patient education resources. It was also my way of coping because I liked the creative process; when things were getting challenging, that was my escape.
Just before I left, we finished a board game to help children adhere to their treatment. We made different cards that listed positive and negative situations/actions. Each card would allow participants to either step forward or step back, depending on whether or not they had adhered to the treatment/ situation mentioned on the card.
For example, one card reads ‘I take my drugs every day at the same time,’ and anyone drawing it can move forward 3 spaces.
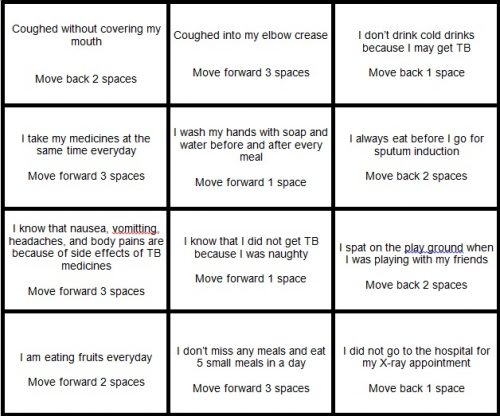
We didn’t want to simply lecture the children, but also engage with them in an age-appropriate way. The game was the best way to reinforce messages we wanted patients to understand.
I also advocated for getting a trained,full-time teacher in the hospital, who could properly address the children’s need for education, help them develop the necessary social skills and motivate them to go back to school. Just before I left, a teaching vacancy was announced in the hospital.
These are changes I am proud to have been associated with. Their treatment would still go on without these changes, but through some of our interventions, we were able to make sure that not all of their childhood was lost to disease. That is immensely gratifying.
In Dushanbe, MSF is working with the Ministry of Health to support a comprehensive care programme for young people with TB and their families. The paediatric TB protocol developed by MSF has been adopted as the national guideline. In 2015, MSF also opened a new project in Kulob, southern Tajikistan, treating paediatric HIV and TB. Medical activities started in the spring of 2016.
Like this story? Or have something to share? Write to us: [email protected], or connect with us on Facebook and Twitter (@thebetterindia).
If you found our stories insightful, informative, or even just enjoyable, we invite you to consider making a voluntary payment to support the work we do at The Better India. Your contribution helps us continue producing quality content that educates, inspires, and drives positive change.
Choose one of the payment options below for your contribution-
By paying for the stories you value, you directly contribute to sustaining our efforts focused on making a difference in the world. Together, let’s ensure that impactful stories continue to be told and shared, enriching lives and communities alike.
Thank you for your support. Here are some frequently asked questions you might find helpful to know why you are contributing?


This story made me
-
97
-
121
-
89
-
167













