After Black Fungus, Now Watch Out For White Fungus; Experts Explain Symptoms
What is White Fungus or Candidiasis? Pulmonologists, Dr Vikas Maurya and Dr Rahul Bahot, answer all your questions about this disease, its prevention and cure.

This article is a part of a series by The Better India to share verified information about COVID-19 care. While several posts on various aspects of fighting COVID-19 are being circulated on social media and messaging services like WhatsApp, we urge you not to trust unverified content. To separate fact from fiction, we will be sharing the videos and content with doctors and experts and bring you their responses with scientific research-backed information.
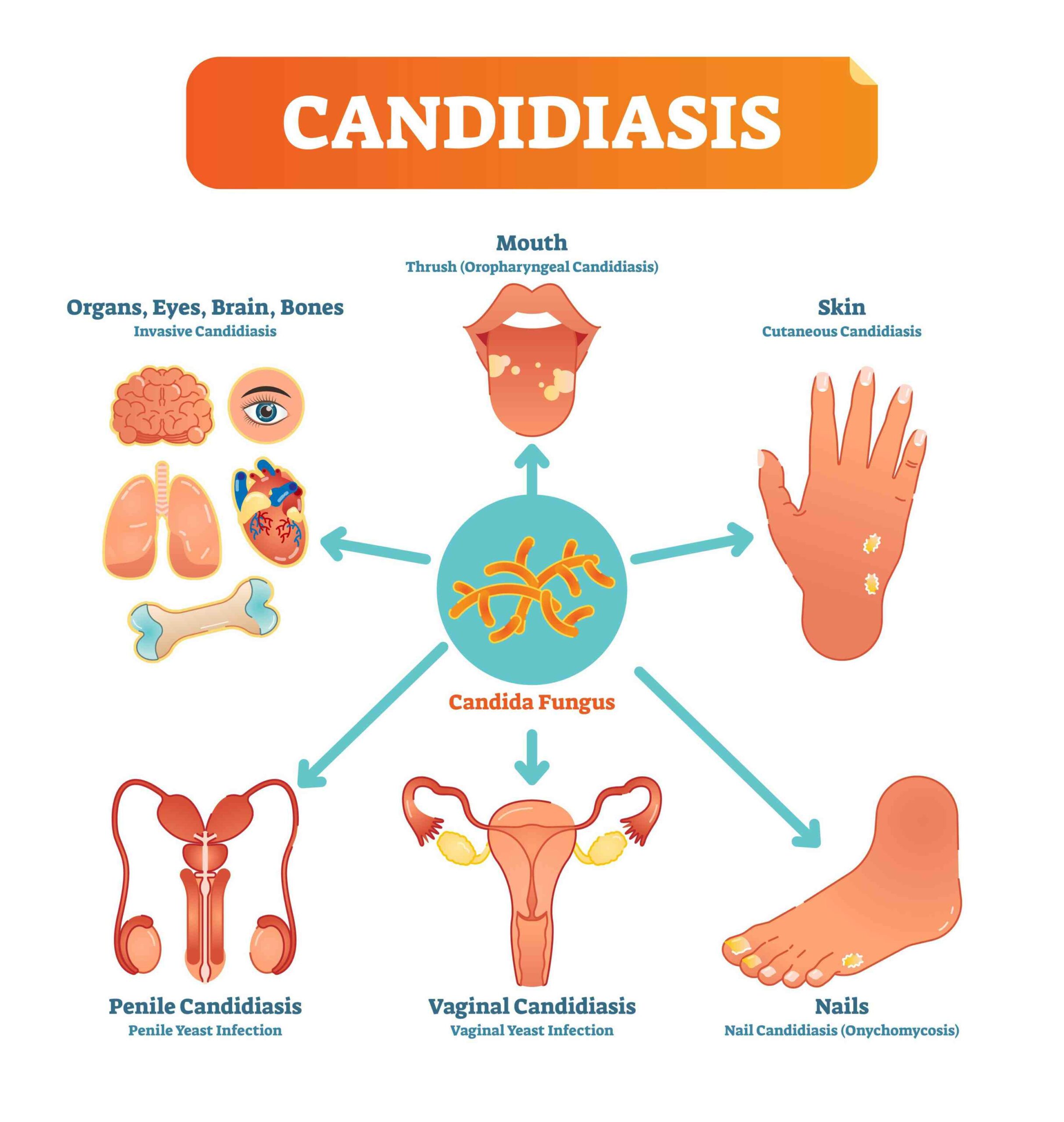
As India sees a spike in Black Fungus or Mucormycosis cases, the medical fraternity has yet another problem to tackle. This time it is being referred to as ‘White Fungus’. White Fungus affects many parts of the body, including lungs, nails, skin, stomach, kidney, brain, mouth and vagina. This type of fungus usually lives on the skin, inside the body and in the environment, without causing any problems.
Dr Rahul Bahot, Consultant Respiratory Medicine and Pulmonology, Jaslok Hospital and Research Centre, and Dr Vikas Maurya, Director and Head of Department, Pulmonology, Fortis Hospital, Shalimar Bagh, answer all your questions on White Fungus and its treatment.

1. What is White Fungus? What are the symptoms to watch out for?
Dr Bahot: White Fungus or Candidiasis is an infection caused by a yeast called Candida. This infection looks like white coloured patches, hence the name. This infection can affect the oesophagus and cause difficulty in swallowing food. White patches are commonly seen around the oral cavity, like the tongue, palate and the oesophagus.
These white patches are visible on physical examination.
Dr Maurya: It is yet another form of fungal infection and is caused due to a compromised or low immune system. Diabetic and cancer patients are at a higher risk of contracting this infection. The infection has been seen in skin, nails, lungs, kidney and even the brain.
We are seeing this develop in patients who have been on steroids as a part of their recovery plan for COVID-19. This is a developing fungus and we are still trying to understand what course of treatment would work best for it. While an anti-fungal will be required, it still requires some research. The mortality rate of White Fungus is currently unknown.
2. Who is at risk of contracting White Fungus?
Dr Maurya: Immunocompromised patients, patients who have been on steroid medication for long, diabetics, cancer patients, patients who have undergone organ transplants and those on immunosuppressant drugs are at risk of contracting White Fungus.
Dr Bahot: Additionally, patients who are prone to asthma and Chronic Obstructive Pulmonary Disorder (COPD), who use steroid-based inhalers and do not gargle post the usage, are also at risk of developing White Fungus.
3. Does White Fungus spread very rapidly?
Dr Bahot: Yes, the White Fungus is of two types – superficial and deep. The superficial one does not spread rapidly, however, the deep fungal infection, which we are currently seeing, spreads very rapidly. Candidiasis is seen in patients who are immunocompromised.
4. How can we prevent White Fungus?
Dr Maurya: The steps to keep White Fungus at bay are similar to what we ask patients to follow for all other infections. Keep your sugar levels under control, do not overuse steroids, ensure that you are taking steroids only under the supervision of a medical practitioner. Follow good hygiene, especially oral hygiene. Always wear a mask given that the White Fungus can spread via spores that can be inhaled.
5. What is the inherent difference between Black and White Fungus?
Dr Bahot: The difference that strikes you immediately is the colour. As the name suggests, Black Fungus is black and White Fungus is white in colour. In terms of their occurrence in the body, Black Fungus takes more immunosuppressants to appear while the White Fungus takes fewer immunosuppressants to show up in the body.
However, during these COVID-19 times, both are rampantly seen given that severe immunosuppressants are being administered to COVID-19 patients. The original source of this White Fungi is Candida, which is in the air, soil and everywhere.
6. Symptoms of White Fungus and Black Fungus are as follows (with inputs from doctors):
White Fungus:
- Cough
- Fever
- Diarrhoea
- Dark spots on lungs and reduced oxygen level.
Black Fungus:
- Headache
- Facial pain
- Nasal congestion
- Loss of vision or pain in the eyes
- Swelling in cheeks and eyes
- Black crusts in the nose.
(Edited by Yoshita Rao)
If you found our stories insightful, informative, or even just enjoyable, we invite you to consider making a voluntary payment to support the work we do at The Better India. Your contribution helps us continue producing quality content that educates, inspires, and drives positive change.
Choose one of the payment options below for your contribution-
By paying for the stories you value, you directly contribute to sustaining our efforts focused on making a difference in the world. Together, let's ensure that impactful stories continue to be told and shared, enriching lives and communities alike.
Thank you for your support. Here are some frequently asked questions you might find helpful to know why you are contributing?


This story made me
-
97
-
121
-
89
-
167














