COVID-19: How India Can Test Fives Times More People While Saving Money & Time
“It can reduce costs and the time taken, and improve the overall efficacy of the turnover time on reports. In that regard, it is a very effective and useful tool,” says Dr Vishal Rao.
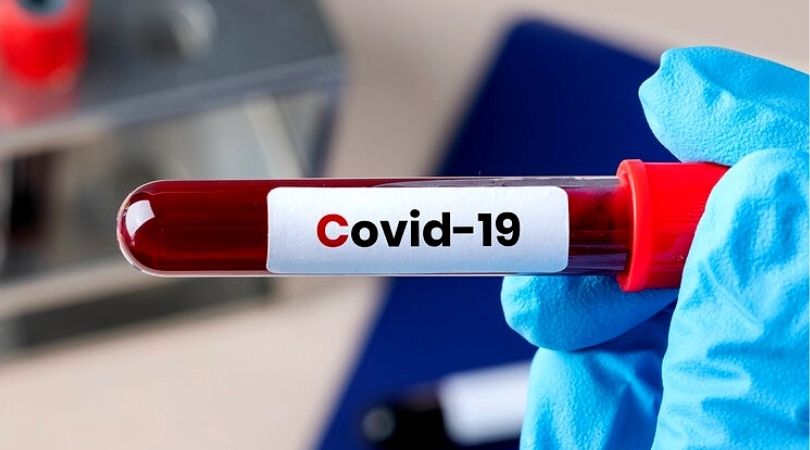
The coronavirus pandemic in India is now growing at the fastest rate in the world. The country has witnessed an increase in cases by 20 per cent since last week with over 1.48 million positive cases. This makes it the third country to have the highest burden of cases in the world after the US and Brazil.
Despite these alarming numbers, testing rates remain low at 11.8 tests per 1,000 people. While researchers and innovators are trying to come up with new kits and technologies to increase the number of samples tested, regulatory approvals can take time. Moreover, the RT-PCR test, the current testing method, is expensive and time-consuming.

As a remedy, researchers have been looking at pre-existing techniques like ‘Pool Testing’, saying how it can reduce costs while being efficient.
What is pool testing?
It is a procedure where samples of various individuals are collected, and divided into groups or ‘pools’; the samples are mixed and tested as one. In case the test is negative, the individuals in the group are cleared, but if the pool tests positive, every person needs to be individually tested.
The Indian Council of Medical Research (ICMR) has already put forth guidelines for how to go about pool testing for COVID-19. As per this, areas with more than five per cent positive cases, health workers who have had considerable exposure and the contacts of individuals who have tested positive are not to be tested using this method. They have also maintained that each pool should comprise not more than five individuals.
The Tamil Nadu Health Minister announced that the state government had approved pool testing in areas where the positivity rate was between 2-5 per cent. Dr. Vishal Rao, the principal investigator from Healthcare Global (HCG), feels that pool testing could work if carried out systematically.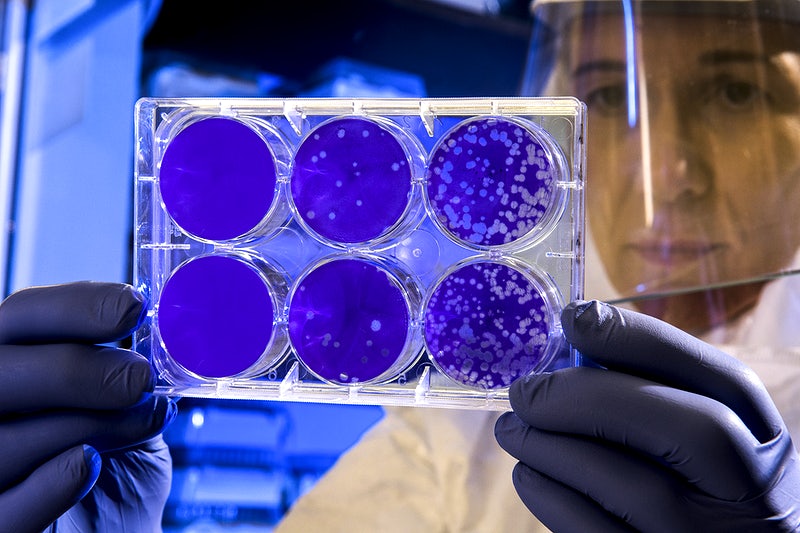
“The important feature of pool testing is that it is an innovative solution to reduce the current burden on the system. It can reduce costs and the time taken, and improves the overall efficacy of the turnover time on reports. In that regard, it is a very effective and useful tool,” he says.
Dr Ravidra Mehta, Chief of Pulmonary and Critical Care Medicine, Apollo Hospitals, Bengaluru, feels that with these tests, “you can rule out a lot of people.”
When the burden on healthcare infrastructure is mounting, can pool testing be the answer? Experts weigh in on how it could be implemented and what to keep in mind.
How and where could this work?
“There is a science to going about pool testing, and it cannot be carried out haphazardly,” states Dr. Vishal Rao who has been researching multiple therapies for treating COVID-19 patients.
In areas where the contagion has spread to a community level, especially in hotspots and red zones, it may not be a wise idea. Also, he recommends people suffering from influenza-like illness (ILI) and severe acute respiratory infections (SARI), to be tested individually.
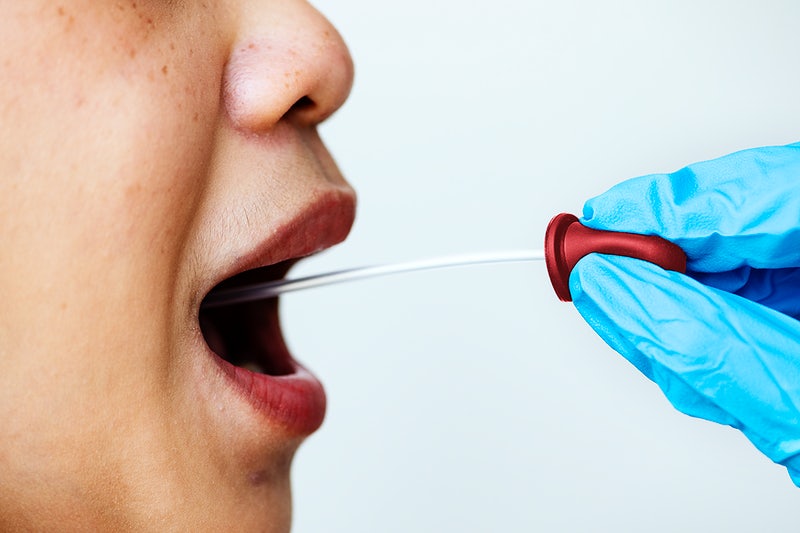
But, the benefits should not be ignored.
“Over 80 per cent of hospitals are checking each patient for every routine procedure. Now, when you test these people individually, and they all turn out to be negative, you end up prioritising everyone equally. When in fact, the focus should be on quickly testing patients who show ILI and SARI symptoms,” says Dr. Rao.
He adds that grouping these incoming patients in terms of their risk of exposure, symptoms, age, and other co-morbidities could be an excellent way to implement it.
“Even when you are using the pool technique, you have to use logic, and you cannot go about it blindly. Always prioritise patients who are at risk and test them individually. Also, even if a pool test comes as a positive, first re-test those who are most vulnerable (old or co-morbid individuals in the pool) susceptible to the virus,” he says.
Dr. Ravindra Mehta feels that this method could save time as you would be grouping individuals who have the lowest probability of testing positive in a pool. The only downside to this, however, is that there might be instances of false negatives, he points out.
“So, if you are taking a group of five, any patient with a low viral load may not be detected, giving a false negative result. But, if one has a low viral load, it is unlikely that they are going to be a spreader, and by definition, super spreaders cannot have a low viral load. At this point, it will help screen the asymptomatic to rule out prevalence in the population by and large,” informs Dr. Ravindra.
He adds that places like community old-age homes with low exposure or rural areas where the burden of positive cases is low can be useful.
“In rural areas where the incidence of cases is low, and the only possibility of community transmission is from rural folk who have migrated back home. If one wants to make sure that there are no chances of community transmission while also hoping that the economy can be jump-started, pool testing can be helpful,” he says.
Both experts emphasise the importance of relying on data sets while employing this method.
“In every aspect of innovation, science has to be the denominator, and one should rely on data along with technology for a balanced approach,” says Dr. Vishal Rao.
(Edited by Shruti Singhal)
This story made me
- 97
- 121
- 89
- 167
Tell Us More
We bring stories straight from the heart of India, to inspire millions and create a wave of impact. Our positive movement is growing bigger everyday, and we would love for you to join it.
Please contribute whatever you can, every little penny helps our team in bringing you more stories that support dreams and spread hope.



















