How Bengaluru’s Methods Can Help India’s Metros Tackle COVID-19 Effectively
"The leaders stood behind the scientists, doctors, researchers letting them do what they know best. This is the ideal way to implement the pandemic protocol," says Dr. Vishal Rao.
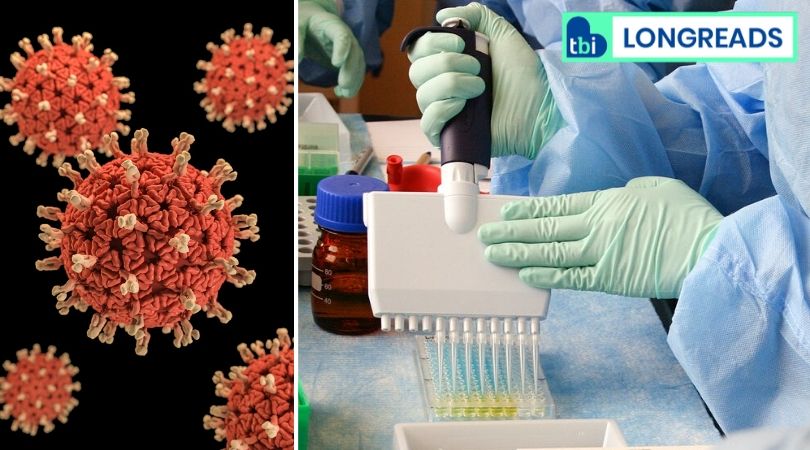
When the pandemic arrived at the start of 2020, it came without any warning. And now, six months into the year, it feels like an uninvited guest overstaying its welcome. Perhaps, no one had anticipated the magnitude of transmission.
I, for one, never thought we would be affected by it. But like many others, I was wrong.
The first case in India was reported on January 30 in Thrissur, Kerala. Over the next few days, the number of positive cases began to rise. Soon, it spread a wave of panic, and all of us began to ask one question, “How do we fight the unknown?”
As of June 9, India recorded 2.66 lakh positive cases, making it the fifth-worst affected country in the world. Government sources reveal that out of these, about 129,917 cases are active positive cases, while 1,29,215 people have been cured/discharged/migrated so far. And, about 7,466 people have succumbed to the disease.
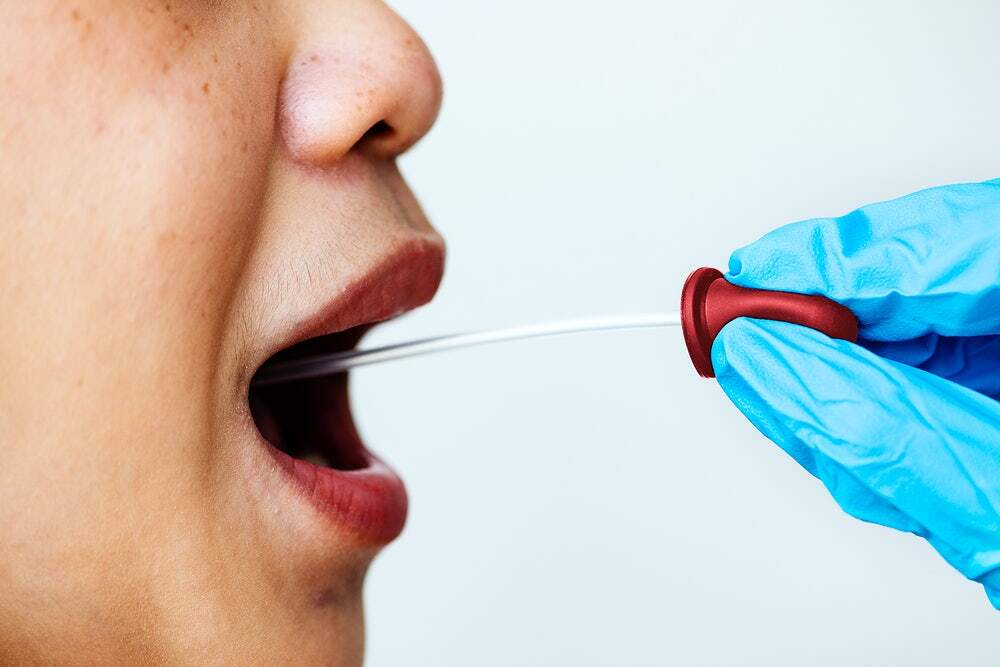
When it came to the spread of COVID-19, metros became the hotspots of transmission. A news report published yesterday spoke about how four Indian cities–Mumbai, Delhi, Kolkata and Chennai–accounted for 50 per cent of the COVID-19 infections in the country.
If you look at Maharashtra itself, there are 88,528 positive cases, surpassing China’s 83,040. Mumbai alone reported about 50,000 positive cases.
But one city stood out in its fight against this novel coronavirus–India’s Silicon Valley, Bengaluru.
With a population of 1.2 crores, the city recorded 501 COVID-19 cases and 19 casualties. On the other hand, the total cases in Karnataka stand at 5,213.
So, what did Bengaluru do right?
We look at a few points that helped Bengaluru manage its rate of transmission and how this approach can be an example for other cities and states. We also look ahead as Phase I of the “unlockdown” or ‘Unlock 1.0’ begins.
Moving into swift action
Dr Giridhar Babu, a member of ICMR’s research task force, says that more than 50 per cent cases in the country are reported from metros. Naturally, whatever load Karnataka had should have come from Bengaluru, but this wasn’t the case.
The 44-year-old, who was a member of the Technical Advisory Group, says that it was the seamless coordination between different stakeholders and the independence given to technical experts like doctors and researchers, that led to Bengaluru’s success. This is also a success for the state.
Dr Vishal Rao, a part of COVID-19 Consultative Group, an independent think-tank, and principal investigator from Healthcare Global (HCG), reiterates the sentiment. He states that the Karnataka government’s approach can be defined by the ‘Wolf Pack Theory’.
“The theory is based on the philosophy that leaders have to lead from behind and not from the front. Meaning that they must help the scientific community lead the war. The leaders stood behind the scientists, doctors, researchers, letting them do what they know best. This is the ideal way to implement the pandemic protocol,” says the principal investigator from HCG.
Bengaluru reported its first COVID-19 case on March 9. Dr Rao informs that by March 10, the COVID-19 Consultative Group, comprising at least 20 experts, reached out to the state government for a clear strategy to deal with what was later declared as a global pandemic.
A few things were very clear. Firstly, the hospitals needed to prepare; they needed sufficient stock of Personal Protective Equipment (PPE) kits, medications, ventilators, hospital beds, and detection kits.
Secondly, a ‘China Wall’ needed to be built to avoid transmission, separating positive cases from the rest of the people. And this required a systematic tracking and testing procedure.
“We meet at least once in two or three days and look at standard operating procedures–the policy on testing, procedure for quarantine, isolation–everything in terms of technical inputs is discussed,” states Dr Giridhar Babu.
He adds that he has “never seen a better, more well-coordinated mechanism anywhere else.”
Tracking, Tracing, and Testing
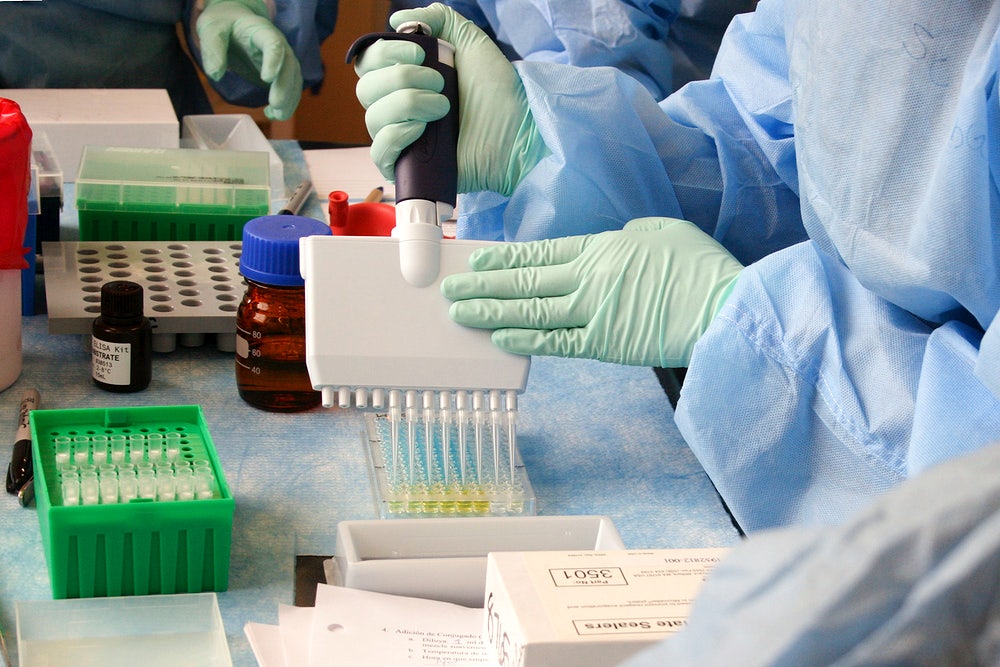
By now, the highly contagious nature of SARS-CoV-2 has been known to us.
“The first person, the techie who got detected, had contact with 2,666 people. It was crucial to track people through contact tracing as 80 per cent of patients are asymptomatic. And hence, it was necessary to track them to build a ‘China wall’,” says Dr. Rao.
And that’s what Bengaluru did.
Dr Babu informs that even before the lockdown, the state Health Department and the Bruhat Bengaluru Mahanagara Palike (BBMP) had procured a list of people who had come to India from high-burden countries.
In most countries, investigations were ‘prospective’, meaning that all close contacts of a patient were tracked down to test, eliminate the possibility of infection, or provide treatment in case of a positive result.
However, Japan and Bengaluru followed a different approach. They adopted ‘retrospective’ contact tracing, following the leads like a detective to find the source of infection. This way, they could document the chain of transmission and trace clusters of people related to one source.
Another approach was called ‘Syndromic Surveillance’. Here, anyone who showed influenza symptoms like cough and cold was traced.
To identify these cases, medical stores were advised to note the information on people who were buying medicines for the treatment of influenza and Severe Acute Respiratory Illness (SARI). And on April 15, the Karnataka government decided to test all these people.
Extensive testing helped detect cases along with better public health surveillance.
“Bengaluru reports one of the highest Influenza-like Illnesses (ILIs). This does not necessarily mean that we have the highest number of cases but shows that we report them better. Also, the testing rates may have improved in other states, but since the beginning, Bengaluru tested 3,500 per million people. This is one of the highest rates of testing, helping in early identification of positive cases,” says Dr Babu.
Letting Science take the lead

Science has played an extremely important role in dealing with the enigmatic Coronavirus, whose several features continue to be a mystery. However, it is the vigour of researchers, scientists, and doctors, backed by the state machinery, that helped in discovering and devising ways to deal with it.
Here, two unique therapies are being discussed–the Convalescent Plasma Therapy and Cytokine Therapy. Dr Vishal Rao was at the forefront of carrying out the clinical trials (Phase-1) for both.
In the initial meeting of March 10, the COVID-19 Consultative Group briefed the ministers about this treatment. The health minister asked doctors and researchers to apply for permission to carry out the clinical trials.
This required coordination between the central government, the Drugs Controller General of India (DCGI), Indian Council of Medical Research (ICMR), along with clinicians. “It is a complex, long process, with multiple reviews and scrutinies and discussions,” informs Dr Rao.
With the help of the state government, Dr Rao and his team of researchers got Elsevier, Lancet’s resource center, onboard.
“They came as an academic partner to support our work and bombarded us with research material proving why we should aggressively pursue clinical trials for plasma therapy. Which is why we were at that stage a month later,” informs Dr Rao.
Convalescent plasma therapy is a treatment used previously for Swine Flu and the Ebola virus. Here, the plasma (blood with red cells, white cells, and platelets removed) of a convalescent (a person who has recovered from the illness) is used, as they have the antibodies that can fight the virus.
Bengaluru was one of the first cities to administer the clinical trial at Victoria Hospital with Dr Rao at the helm. So far, the treatment has been administered to two people.
The first patient was admitted on May 10 and was extremely critical which is why he was put on a ventilator. On May 12, they decided to administer plasma therapy as his condition was rapidly deteriorating. In 48 hours, he showed signs of recovery. But, because of his history of cardiac disease, diabetes, and hypertension, he suffered cardiac arrest.
“Almost 86 per cent of patients on ventilators do not make it, and unfortunately, this patient had complications because he was a heart patient. But, the second patient who was also critical, responded positively. They have been discharged from the ICU and moved to the ward as we speak,” informs Dr Rao.
Dr Gururaj Rao, a Cell and Molecular Biologist, and Dr Jythosna Rao, an Immunologist, have been working with Dr Vishal Rao on their study for Cytokine therapy. The clinical trials for this therapy began as per government guidelines last week on six healthy persons.
“I am happy to inform you that these healthy persons, who were administered the injections, are doing fine, and this has given us a lot of hope,” he says.
Strict implementation of guidelines

With the pandemic, there came a need to set out proper guidelines to control the rates of transmission. Law enforcement agencies like the police played a vital role in the implementation.
Isha Pant, DCP, Command Centre and former nodal officer in Bengaluru for the COVID-19 outbreak, discusses how the police worked round the clock to ensure that strict guidelines were followed by city dwellers.
Any area with even a single positive case was declared as a ‘containment zone’, and all roads leading to it were blocked. DCP Pant shares how police officers worked 24 hours in three shifts, surveilling these zones, ensuring that there was no entry and exit in these areas without permission (except in case of medical emergencies).
Additionally, 200 check-posts around the city further monitored the movement of people, and passes were only given to essential workers.
Home quarantine was also strictly followed after contact tracing. “The police went door-to-door along with BBMP officials. We got a list from the health department, which procured a list of travellers from the airport. We were successful in ensuring about 20,000 people who had travelled to foreign countries, were home quarantined for 14 days as per guidelines,” she says.
For this, they also issued notices to Resident Welfare Associations (RWAs) and neighbours, and those asked to home quarantine had marks on their fingers with the same ink used during elections.
With help from BBMP and volunteers, social distancing markers were drawn across the city. About 272 police patrol vehicles, commonly known as Hoysalas, were helping people (the elderly, pregnant women, and others) move around in case of emergencies.
Additionally, the safety of police personnel on duty was also prioritised. This is why regular tests were conducted for the police personnel, who also had access to face shields, sanitisers, and masks.
Major learnings and the road ahead
When it comes to dealing with the novel coronavirus epidemic, nothing is certain, feels Dr Babu. One cannot always follow a strategy, especially when situations are constantly evolving. But he does give a few pointers that can be helpful in containing the spread.
“Firstly, religious gatherings can be major hotspots for something as contagious as COVID-19. And I feel state governments should ensure that such places remain closed, as these institutions are visited by high-risk groups like the elderly,” he says.
The second point he highlights is strict quarantine measures for domestic travel (seven days institutional quarantine and 14 days of home quarantine after that), especially for those who travel from high-burden states like Maharashtra.
For Dr Vishal Rao, the pandemic has been a big lesson in taking affirmative action.
“The definition of time has changed during this crisis, especially in the scientific world. Scientific research can take as long as 17 years to move from the lab to the practice. But, this pandemic has taught us that in crucial times, it can be narrowed down to 17 days. Look at how we have swiftly administered the clinical trials,” he says.
Dr Rao also talks about the importance of data in the current context. The COVID-19 Consultative Group, which he is a part of, comprises experts and data scientists working with international experts from Harvard School of Public Health and Elsevier. Their findings can pave the way for future actions and deliberations.
- Protect the elderly
From their data sets, they found that the most vulnerable group that caught the virus was between the ages of 20-40 years. However, the fatal group comprised people above the age of 65 and those who are immunocompromised due to underlying non-communicable diseases.
“In such a situation, we need to follow the measures of ‘reverse quarantine’, where we protect these people. It is the individual’s responsibility to protect the elderly and the immunocompromised. This is why I say that this is a war we need to fight from home,” he emphasises.
- Don’t ignore non-communicable diseases
“We have found that the virus is specifically dangerous for those who suffer from underlying non-communicable diseases of the heart, lung, diabetes, hypertension, cancer, chronic obstructive pulmonary disease (COPD), among others. And most of the deaths are in this comorbid group,” he informs.
Increasing awareness about these high-risk groups can help in taking proper preventive measures and strengthening their weak immune systems.
- Reverse mentoring
Students and scientists should engage in research against COVID-19, says Dr Rao.
“This is the time when we exchange ideas and innovate. We have already hosted innovation challenges that involve clinicians, engineers, students, and researchers so that we can find a solution and contain this virus together,” he says.
Although this novel coronavirus may have brought the world to a standstill, Dr Rao believes that this pandemic is a lesson we must not forget.
“Amid capitalism, communalism, corruption, and global warming, the coronavirus has evoked a sense of humanism and given a big push to innovation. It has shown us the power of science and the human spirit. We cannot go back to our old ways. It is time to see the world through a fresh pair of eyes,” he says.
Maybe Dr Rao is right. Perhaps that is the only way forward.
(Edited by Shruti Singhal)
Like this story? Or have something to share?
Write to us: [email protected]
Connect with us on Facebook and Twitter.
This story made me
- 97
- 121
- 89
- 167
Tell Us More
We bring stories straight from the heart of India, to inspire millions and create a wave of impact. Our positive movement is growing bigger everyday, and we would love for you to join it.
Please contribute whatever you can, every little penny helps our team in bringing you more stories that support dreams and spread hope.



















