Nipah to Coronavirus: IAS Officer Explains Why Kerala Is Better Prepared Than Most
“The first lesson Kerala’s state apparatus learnt during the Nipah episode was to never underestimate the extent of a potential epidemic”, says Dr Rajeev Sadanandan, retired IAS officer and the brain behind Kerala’s successful arrest of the Nipah virus. #CoronavirusPandemic

The Kerala government has received widespread praise for how it has proactively handled the Coronavirus (COVID-19) epidemic. From holding daily briefings on the virus, ensuring better access to practical information for the general public to inculcating best public health practices in times of epidemics like rigorous contact tracing and maintaining strict protocols for quarantining, the Kerala government has so far managed to keep the number of confirmed positive cases to 27, including 2 foreign nationals, with no fatalities.
Earlier this week, The Better India spoke to Dr Rajeev Sadanandan, the former Health Secretary of Kerala, who played a critical role in the government’s successful efforts to contain the Nipah virus, about the lessons learnt from previous disease outbreaks and how it’s implementing them in their current battle against the novel coronavirus.

A brief timeline
Back in January, preparations to take care of the 26 medical students coming from Wuhan, China, the first major epicentre of the virus, had begun in earnest. The government knew who these students were before they landed in the state. These students were quarantined and regularly tested. Among them, three had tested positive and were treated.
Unfortunately, more epicentres emerged in East Asia, Europe and the Middle East. Suddenly, the number of people who could potentially carry the infection to Kerala went up exponentially. So, the State Health Department continued to track people coming in from this region, ensuring that they were isolated and treated.
In an act of carelessness, however, one family (a couple and their 26-year-old son) did not inform the health authorities about their recent trip to Italy. Even when they had the infection, they had failed to inform the health authorities.
After quarantining them, health workers in the state retraced their steps on war-footing and found 3,000 people who they had come in contact with since landing in Kerala. Among the 3,000, they found six more positive cases. Now, they are retracing their steps and their contacts are being identified.
In other words, the second wave of COVID-19 outbreak in Kerala began with the carelessness of that one family. With positive cases flying in from different corners of the world since, the total number stands at 27.
Coronavirus has not been contained, but governments must ensure that the number of those affected and casualties remain as low as possible. What the Kerala government hopes to do is ensure that peak numbers remain as low as they can. How is that being done?
“It’s by using classic public health techniques. Unlike Nipah, the epicenter of the epidemic was known. The advantage is that you know where carriers of the virus are coming from. People under low risk of contracting it can be put under home quarantine, while a health worker follows up with them morning and evening. This was a technique developed during the Nipah outbreak,” Dr Rajeev Sadanandan tells TBI.
Now, if a person tests positive, what ensues is the painful process of tracing and identifying their contacts for the previous 14 days. Their steps are retraced with answers to questions like: Which flight did they take, their seat number, the immigration officer they met, the taxi driver who ferried them, whether they stopped at a restaurant to have a cup of coffee or visited a shop, and who they meet and dine with, etc.
“Upon their admission in the hospital, we begin tracing their past movements by interviewing them, their relatives, mapping their movements by tracking their mobile phones using cell tower triangulation, Google Maps, identifying which places they visited and cross-checking it. We mark each and every point they visited,” says PK Sudheer Babu, the District Collector of Kottayam.
“And that cycle starts again because every person who the patient came in contact with could become the centre of the next cohort of potentially virus-affected persons. This could go on until a point where it impossible for the Health Department to keep following up. By then, the numbers are so large that you step away from prevention and immediately get down to mitigation. I’m not sure when that stage arrives, but I believe the government is ready for it,” adds Dr Sadanandan.

Lessons learnt from Nipah
According to him, the first lesson the State apparatus learnt during the Nipah episode was to never underestimate the extent of a potential epidemic. “The reaction to the Nipah virus, for example, was way above the then available threat perception,” he says.
The second key lesson was establishing a robust contact tracing mechanism, which is something they learned during the two Nipah episodes. Contact tracing is a standard public health practice in managing any infectious disease.
The local Multipurpose Health Worker (MPHW), including Auxiliary Nurse Midwives (ANMs) and multipurpose male workers, track down primary and secondary contacts, who are then home quarantined. The assigned MPHW calls them up in the morning and evening to ascertain whether they have developed any symptoms, while a trained psychologist inquires about any psychological issues arising from the quarantine.
Meanwhile, low-income families under quarantine receive free rations. If any patient under quarantine reports any symptoms, they are presumed to be a Covid-19 positive case. They are then transported in designated ambulances to the isolation ward in the designated treatment centres and tested. Until their test results are negative, they remain in isolation.
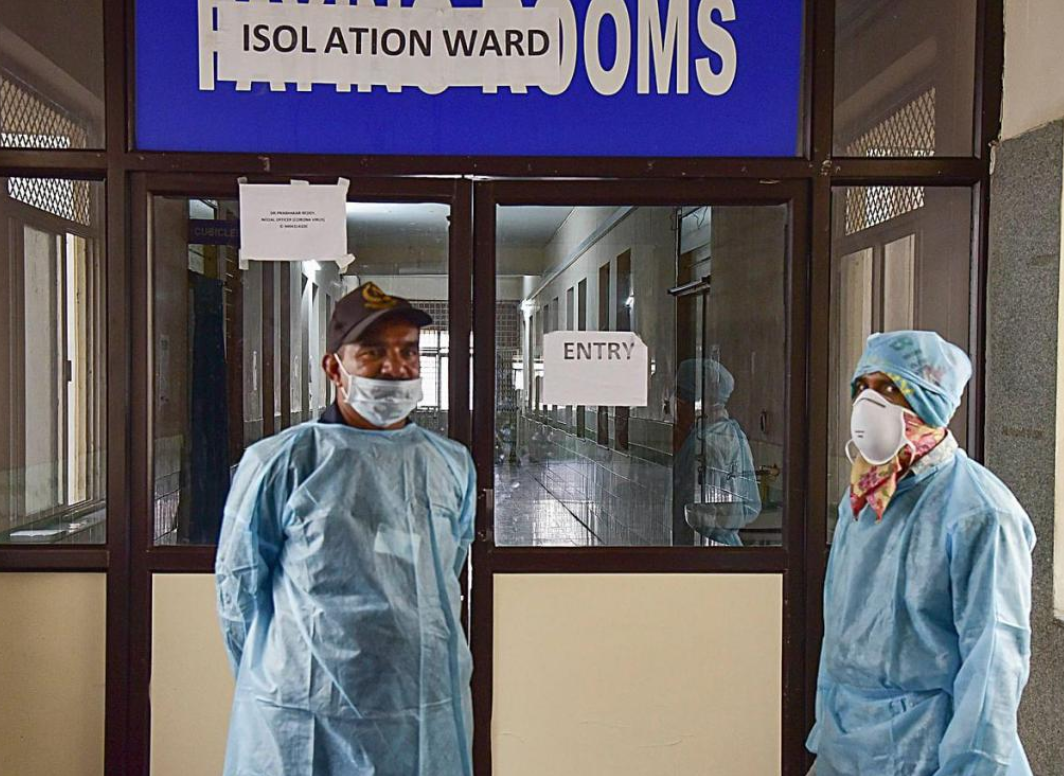
“Over time, these MPHWs have learnt this process of how to conduct contact tracing, how to figure out the next potential cohort, how to follow up on them, and how to shift them to a medical centre if they transition from low to high risk patients. These health workers are trained professionals when it comes to dealing with these situations. They were first trained during the first Nipah episode, and ever since it has become part of the standard training given at the district level,” informs Dr Sadanandan.
Ideally, those with symptoms would normally report themselves to the authorities along with their contact number and their address. All that information is relayed to the said MPHW concerned, who tracks the quarantined patient.

Health workers following up on people under quarantine. (Source: Twitter/Sneha Koshy)
The process of contact tracing is incredibly difficult, and it is likely that some cases will get missed. But can they reduce the number of cases missed? If any of them tests positive, can they recover from a bad situation fast enough like in the case of the couple returning from Italy?
“Thankfully, it was an alert physician who picked it up not from the infected couple that flew down from Italy, but another person they had infected. To the credit of the Kerala government, they cracked down so fast that only six positive cases have emerged including the couple from that episode. Among the 6, one was 91 years old. The other was 86 years old, and it would have been very difficult to save their lives. Incredibly, they have recovered. That’s quite an achievement.
In fact, I was very surprised because if you look at cases from Wuhan and Italy, one would surmise that the probability of their survival was very low. Now, their contacts are being identified. The health department is now straining itself to identify all their contacts, monitor and check whether fresh positive cases are coming up to ensure the virus doesn’t set roots in the state,” claims Dr Sadanandan.
If anyone was here in the given place, date and time plz contact nearest health facility #coronavirusindia @ pic.twitter.com/MRCgEiiaMU
— Navjot Khosa IAS (@navjotk28) March 10, 2020
Another key lesson from the management of Nipah was the realisation that the State government couldn’t manage the response by itself. Support for contact tracing is largely mobilised by robust local self-government entities like Panchayats and urban local bodies. NGOs, meanwhile, have arranged for the supply of protective gear. Religious leaders, civil society members, media and opinion drivers in the state are co-opted to further the government’s efforts in battling the virus.
It was also during the Nipah outbreak when the State government really built up its presence on social media to not merely answer questions, but also counter fake news. Those intending to spread panic via fake news were subject to punitive measures.
Also Read: Exclusive: Despite Mom’s Appeal, Indian Doctor Stays Back to Save Lives in China
The Challenges Ahead
“One thing we learnt from Nipah and the MSF (Médecins Sans Frontières) guidelines on Ebola management is to isolate positive cases at source. What we did during Nipah was to take a seperate building inside the Kozhikode Medical College premises, which was an epicentre of the outbreak. All suspected cases or those who reported respiratory distress or acute fever were asked to report to that facility rather than the general outpatient department of the hospital,” recalls Dr Sadanandan.
Any person with symptoms would be driven there directly on government expense. If these cases warrant admission into the facility, they would do it. There were four levels to this building inside the Kozhikode Medical College campus with each carrying different patient segments—suspected but not confirmed cases or confirmed but not serious cases.
“Now, the number of COVID-19 cases is going to be much higher than Nipah. They would have to look at alternative strategies like hiring a stadium. Each district may need a separate such structure to house patients. Also, based on their experience of the 2018 floods in Kerala, the State government realized that they need more boots on the ground in dealing with such emergencies. They have decided to recruit additional people, train them and keep them ready for any possible spike in the spread of COVID-19,” he claims.
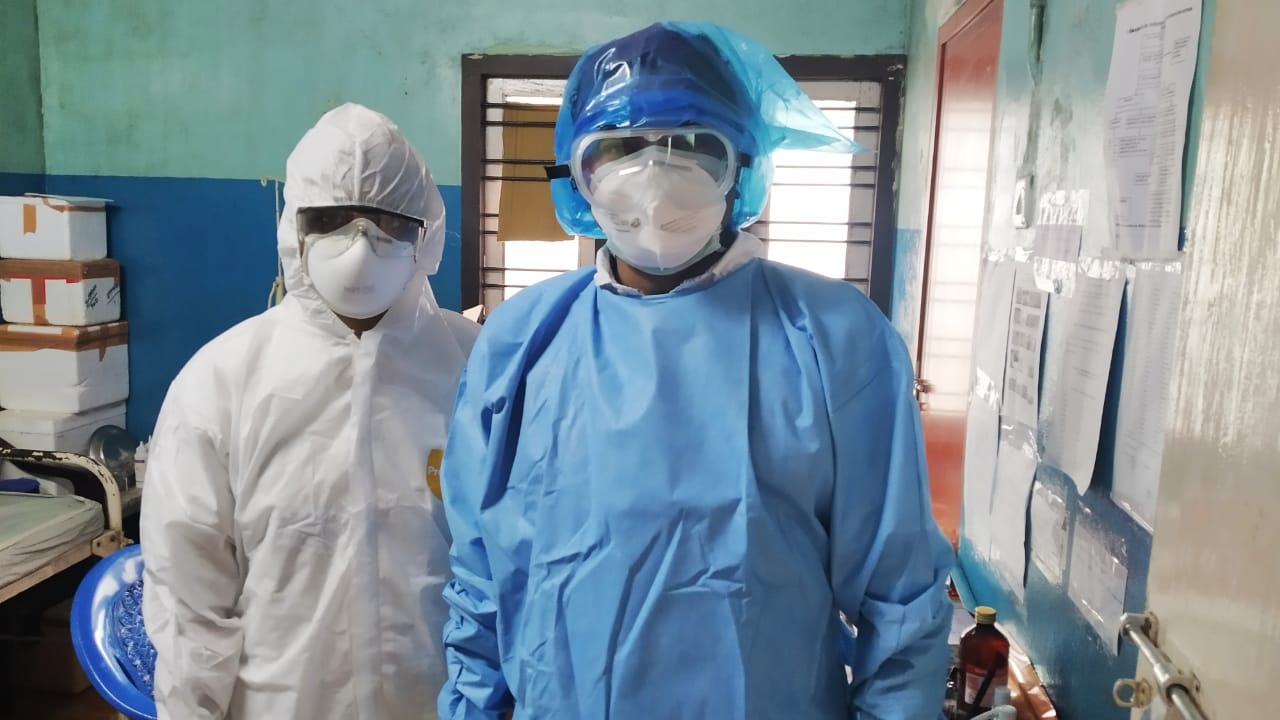
Another serious concern is the possibility of widespread community transmission.
“Since symptoms are indistinguishable from common conditions, cases would get ignored and till they become severe and the infection has spread to the larger community…Community spread would involve older patients who are at higher risk…Creating the facilities takes time. Government may need to identify buildings, procure oxygen cylinders, masks, cannulas and ventilators and recruit personnel immediately. This may at worst be wasted effort. But if support is needed and not provided, it could lead to avoidable deaths, loss of morale of health and anger in the community,” he writes for the Observer Research Foundation.
There is also the issue of mass testing, and many commentators believe India is not doing enough. However, earlier this week, R Gangakhedkar, the head of epidemiology and communicable diseases at the Indian Council of Medical Research told the press, “We have not yet reached the stage of mass testing, where the virus spreads unfettered in the community. We are at Stage Two of local transmission.”
The ICMR had also announced an expansion of their testing process, while encouraging private players to test patients.
Meanwhile, as responsible citizens, people must inform medical professionals if they have arrived from a COVID-affected country, be honest about whether they’re suffering any symptoms and take all necessary precautions to ensure they don’t infect others.
This will go a long way in helping health workers on the frontline.
(Edited by Saiqua Sultan)
Like this story? Or have something to share? Write to us: [email protected], or connect with us on Facebook and Twitter.
This story made me
-
97
-
121
-
89
-
167
Tell Us More
We bring stories straight from the heart of India, to inspire millions and create a wave of impact. Our positive movement is growing bigger everyday, and we would love for you to join it.
Please contribute whatever you can, every little penny helps our team in bringing you more stories that support dreams and spread hope.



















