Bangladeshi Doctor’s ‘Life-Saving Shampoo Bottles’ Will Help Us Battle Pneumonia!
The findings of the year long experiment showed a 75% decrease in the death rate of pneumonia-affected children who used the device.
Ask doctors about the most harrowing part of their job and the usual reply would be losing a patient under their care. For Dr Mohammod Jobayer Chisti, losing three children to pneumonia on his first night shift is a horror he hopes no other doctor suffers.
Sylhet MAG Osmani Medical College Hospital, Bangladesh, 1996: Young Dr Chisti was working his night shift in the Pediatrics department. The ward was grim as 20 children were being treated for pneumonia.
Despite Dr Chisti’s best efforts that night, the condition of three children declined rapidly, not to recover.
“I felt so helpless. I was thinking what the point of studying medicine was. I felt that we had missed out on something, but we were unsure about what that was. Maybe it was a lack of knowledge or insufficient resources,” Dr Chisti said to Dhaka Tribune.
Pneumonia is one of the leading causes of death for infants around the globe. It is the result of an infection in the lungs which could be bacterial, viral or fungal and is usually seen in children below the age of five. The infection makes it difficult for the patient to breathe.
Though procedures are available, it requires expensive equipment like ventilators, which not every hospital can’t afford. A single ventilator can cost upwards of Rs 10 lakh, which is why poorer hospitals use a face mask or makeshift tubes and place these near the nose of the patient. This method, though useful for healthier children, might not work with pneumonia-affected kids.
But instead of being consumed by the experience, Dr Chisti made it his mission to fight for an affordable and better treatment for children and families with below-average incomes.
He finished his MD in paediatrics and children’s lung function from The Royal Children’s Hospital in Melbourne, Australia, in 2012, and joined the International Centre for Diarrhoeal Diseases Control, Bangladesh (ICDDRB).
It was here that he made a device to make breathing easier for pneumonia patients. And what’s more, his solution used shampoo bottles!

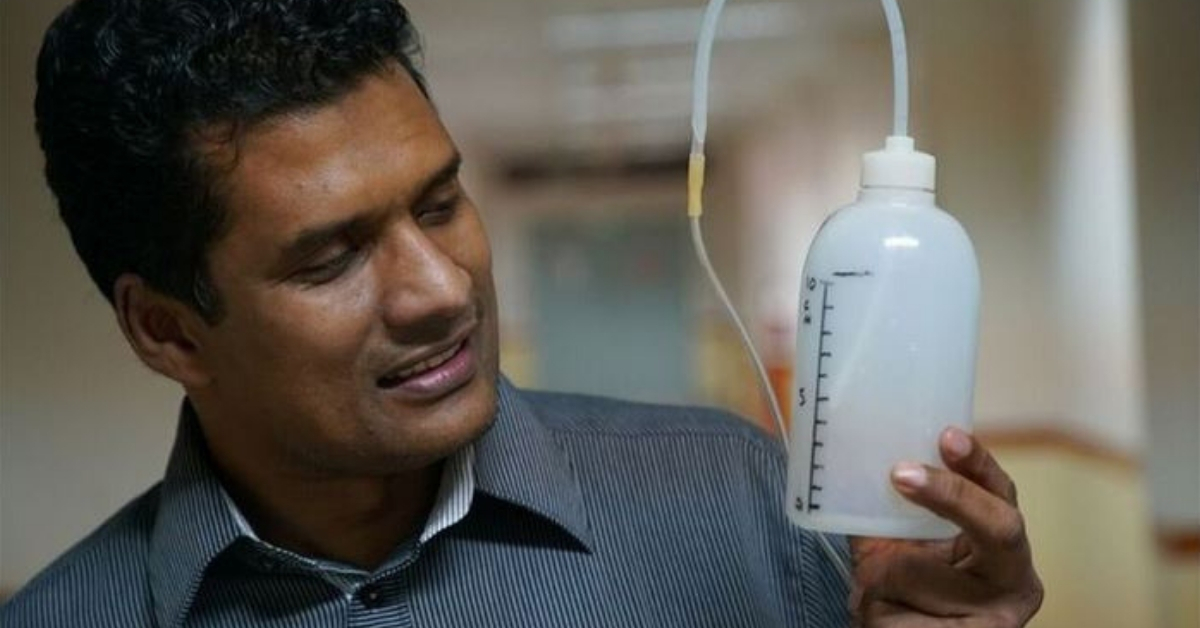
Using an oxygen supply, usually provided from the face mask, some tubing and a plastic shampoo bottle filled with water, he was able to build a version of a bubble-CPAP ventilator. The bubble-CPAP (continuous positive airway pressure) ventilators channel the infant’s exhalations through a tube, which has one of its ends immersed in water.
The exhaled air bubbles up from the liquid, causing fluctuations in the air pressure of the tube. The rapid pressure changes are fed back to the child’s lungs, stabilising the exchange of carbon dioxide for oxygen. The process requires less effort from them and makes it easier for them to breathe.
“We carried out experiments on some of the children using the medical water bottles filled with water, and a plastic tube inserted into one end. The children then inhaled oxygen from a tank and exhaled through a tube, producing bubbles in the water in the bottles,” Dr Chisti told the publication.
The findings of the year long experiment showed a 75% decrease in the death rate of pneumonia-affected children who used the device. By July 2013, the method of treatment had been in practice at Bangladesh’s International Centre for Diarrhoeal Diseases Control.
Dr Chisti and his team are now ready to take the innovation to other countries like Ethiopia, where trials will be conducted for implementation.
Kudos to the doctor for innovating a solution which only costs INR 90 to make but could save infants worldwide!
(Edited by Shruti Singhal)
Hey, you may also like: When The World Stood Aside, Mongolia Backed India In Recognising Bangladesh!
Like this story? Or have something to share?
Write to us: [email protected]
Connect with us on Facebook and Twitter.
This story made me
- 97
- 121
- 89
- 167
Tell Us More
We bring stories straight from the heart of India, to inspire millions and create a wave of impact. Our positive movement is growing bigger everyday, and we would love for you to join it.
Please contribute whatever you can, every little penny helps our team in bringing you more stories that support dreams and spread hope.



















