As Indian Women Line up to Get New Wombs, Here’s All You Need to Know About Uterine Transplants
“In our country parents will go to any lengths to ensure that their daughter can have a baby.”

India’s medical fraternity has watched with caution as a Pune hospital conducted a successful womb transplant, the first surgery of its kind in the country. With the success of this procedure, sources at the hospital say that more than 20 women have already come forward to undergo the procedure that can enable them to bear children.
In India, the primary legislation dealing with organ donation and transplantation is the Transplantation of Human Organs Act, 1994. The Act aims at regulating the removal, storage and transplantation of human organs for therapeutic purposes and prevention of commercial dealing with regard to the organs.
Dr Uma Ram, a Chennai-based gynaecologist and obstetrician says, “From a medical perspective it is quite an achievement. Any organ transplantation is a very complex procedure. The fundamental difference between uterine transplant and other organ transplants, like a renal or liver is that uterus transplant is not essential for life. Whereas renal and liver transplants are done when there is an illness that can potentially take away life.”
“Uterine transplant is to give the woman the ability to procreate.”

According to statistics, 1 in about 5000 females is born without a uterus, while the others interested in this procedure are women who have had to undergo hysterectomy due to cancer or other medical conditions. One must make note of the fact that a woman who undergoes the uterus transplant will not be able to conceive naturally since the fallopian tubes, that usually carries the egg to from the ovaries to the uterus, cannot be connected. Once the transplant is successful, the recipient will have to rely on IVF to ensure pregnancy.
Like other transplants, the recipient must be put on immunosuppressant drugs to ensure that the body does not reject the uterus. The stage at which doctors can deem a transplant successful remains unclear. Is it after the recipient starts menstruating or once the recipient gets pregnant? If the IVF procedure fails, can the recipient choose to keep the uterus? These are questions that haven’t been answered yet, but that are imperative to put forth given the stage at which these transplants are in India.
With this transplant, medical science has certainly made great strides. But as the science becomes more advanced, so does the ethical dilemma. Speaking about the legal implications of womb transplants, Dr Uma says,
“It is too soon to say anything about that. There have to be very strong regulations: which centre can carry out the procedure, who are the women who can accept the transplant and who can donate. These are questions that need clear answers.”
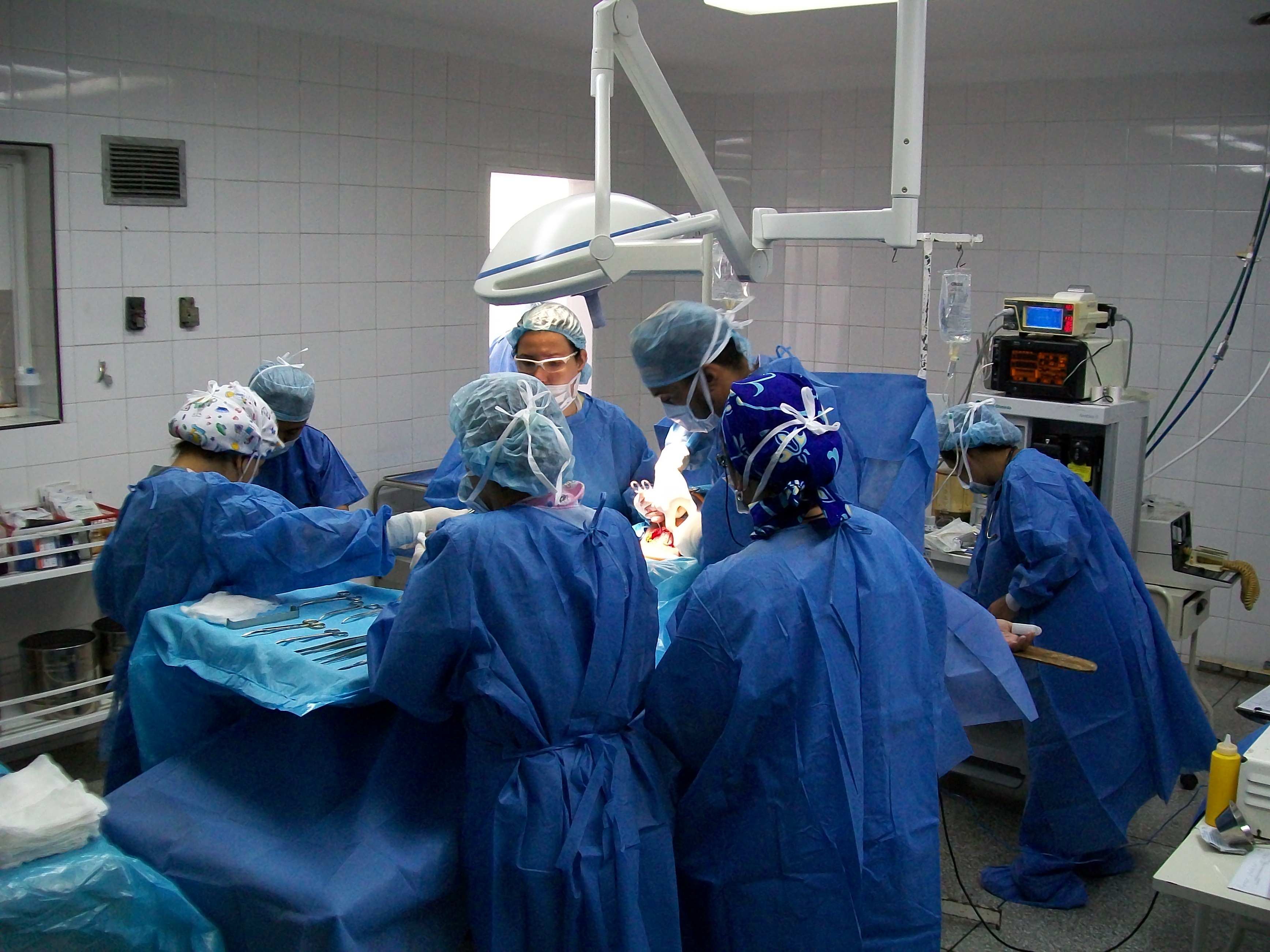
Photo Source: Wikimedia Commons
The first time such a transplant was successfully undertaken was in Sweden, in the year 2013. This was followed by Britain and America. Unlike Sweden where live donors participated in the study, only deceased donors were used in the American study.
The recent transplant was conducted in Pune, after the Maharashtra Directorate of Health Services granted a five-year licence after inspecting the hospital’s infrastructure and facilities in April.
It is important to note that the first successful womb transplant accomplished in Sweden was preceded by 11 unsuccessful attempts by doctors worldwide. Until now, only 6 babies have been delivered after the transplantation.
While benefits of the procedure are yet to be seen, it is imperative that one does a cost-benefit analysis before applauding the move. Dr Uma says, “In our country parents will go to any lengths to ensure that their daughter can have a baby. Which makes it that much more important to have rules and regulation in place for this kind of transplantation.”
Dr. Ankur Garg, a liver transplant surgery consultant at BLK Super Speciality Hospital, New Delhi, says, “The thing with uterus as it stands now is that anyone is at liberty to get it removed, since it does not affect the functioning of the body. Therefore a uterus removal surgery cannot be denied. Insofar laws are concerned, the same laws that govern other organ transplants will be applicable to uterus also.”
Speaking about the safety of such transplants, Dr Ankur says, “Medically the uterus is not a vital organ, so with the transplant the donor is absolutely safe. In cases where the recipient rejects the organ, it just needs to be removed without impacting the functioning of the body.”
“Technically the uterus transplant, vis-à-vis other solid organs like kidney, liver and intestines, is one of the easiest transplants with respect to risk to the patients.”

Photo Source: pixabay
Some important points to note with respect to uterus transplants:
1. The sole aim of uterus transplants is to help women bear children.
2. Women who undergo the transplant will be able to conceive only through IVF and not through
intercourse.
3. These pregnancies have to be closely monitored throughout the term because women will not be able to feel labour pains and contractions once they begin.
4. Once the desired number of children has been had, the uterus will have to be removed.
5. Doctors have to perform an elective C-section on women who have undergone womb transplant
When it comes to children, there is nothing that a parent won’t do. There are often no logical construct or limit, when it is a matter of “my child”. In case of the recent Pune surgery, the donor (the recipient’s mother) was doing it for her child and the recipient is doing in order to have hers.
Amidst the popular notion that women must bear children to be ‘complete’, explaining the pitfalls of procedures like womb transplants might become a challenge. It is important however to realise that, medically and scientifically this is a great advancement, it is important that the donor and the recipient are made fully aware of all the pros and cons of such transplants.
Like this story? Or have something to share? Write to us: [email protected], or connect with us on Facebook and Twitter.
NEW: Click here to get positive news on WhatsApp!
If you found our stories insightful, informative, or even just enjoyable, we invite you to consider making a voluntary payment to support the work we do at The Better India. Your contribution helps us continue producing quality content that educates, inspires, and drives positive change.
Choose one of the payment options below for your contribution-
By paying for the stories you value, you directly contribute to sustaining our efforts focused on making a difference in the world. Together, let’s ensure that impactful stories continue to be told and shared, enriching lives and communities alike.
Thank you for your support. Here are some frequently asked questions you might find helpful to know why you are contributing?


This story made me
-
97
-
121
-
89
-
167













